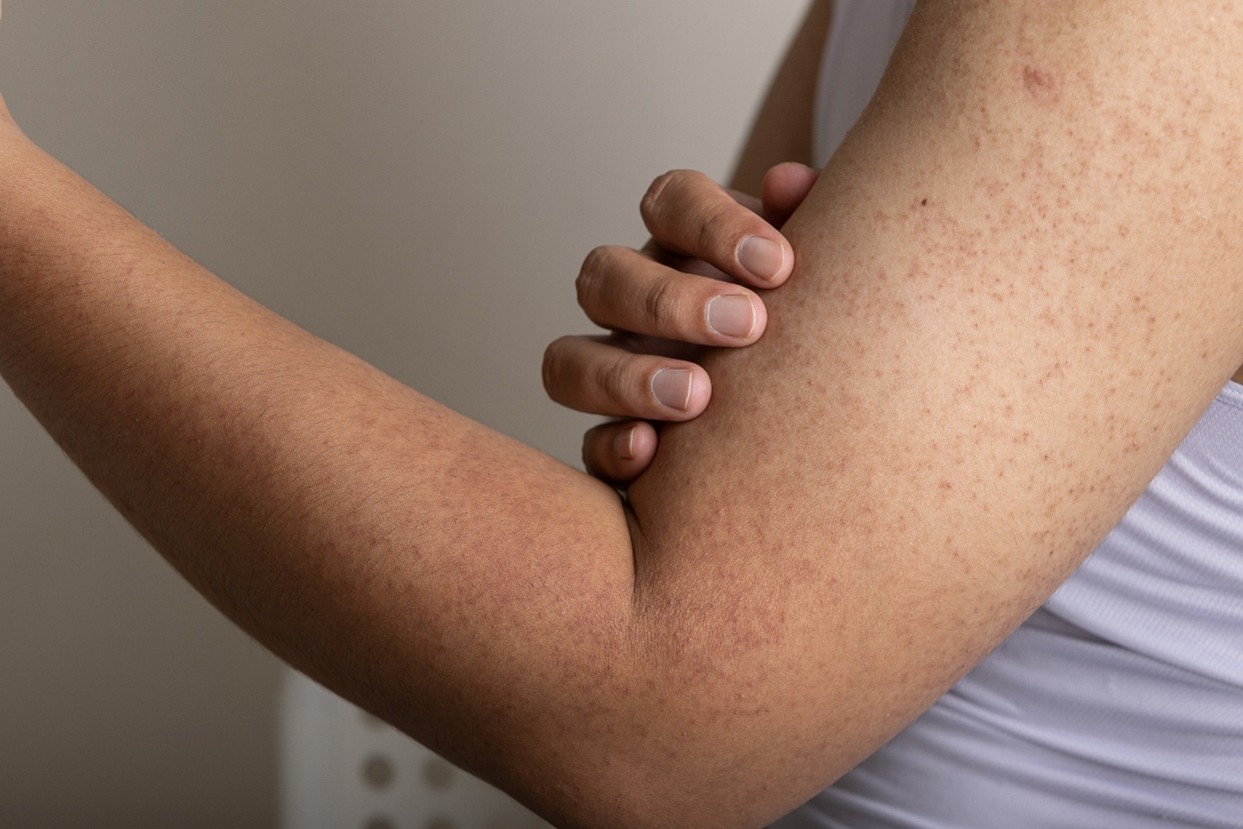
What is keratosis pilaris?
Keratosis pilaris is a common, harmless skin condition that causes small bumps to appear on the skin. These bumps can appear anywhere, but they’re often found on the upper arms and thighs. Some people have so many bumps that they extend onto the forearms or lower legs.
Symptoms of keratosis pilaris
This condition may make your skin look like you have patches of “goose bumps.” The bumps are often the color of your skin. They may also look white, red, pinkish-purple on fair skin, or brownish-black on dark skin. The bumps can feel rough and dry like sandpaper. They may itch, but they don’t hurt. If you have keratosis pilaris on your face, it may look like acne, and you may look flushed. Additionally, the skin on your face may be dry and chapped. Some people with keratosis pilaris only get a few flesh-colored bumps while others have noticeable bumps that can look like a rash.
The area of your skin that is affected by keratosis pilaris may become darker (hyperpigmentation) or lighter (hypopigmentation) than the surrounding skin. This can happen if you scratch or pick at the bumps.
What causes keratosis pilaris?
Keratosis pilaris occurs when dead skin cells clog the hair follicles (also called pores) in your skin. It’s not caused by a fungus, bacteria, or a virus. It’s not contagious. It occurs more often during the winter months when the air is dry, and it tends to improve in warmer months when humidity is higher.
This condition can occur at any age and affect anyone. It usually appears before age 2 or during the teenage years, however it can worsen during pregnancy and after childbirth. Keratosis pilaris generally affects women more often than men, and it may disappear or improve with age.
You are more likely to develop keratosis pilaris if you have:
- A family history of it
- Asthma
- Dry skin
- Eczema (also called atopic dermatitis)
- Excess body weight
- Hay fever
How is keratosis pilaris diagnosed?
Your doctor will be able to tell if you have keratosis pilaris by looking at your skin and talking with you about your symptoms. In some cases, however, your doctor may need to perform a skin biopsy to ensure a correct diagnosis.
Keratosis pilaris treatment
There is no cure for keratosis pilaris. But you can minimize your symptoms by following your doctor’s recommendations. He or she may suggest you:
- Use a moisturizing lotion to soothe your skin.
- Exfoliate your skin. This is when you use a loofah or rough washcloth to gently remove dead skin cells from the surface of your skin.
- Apply skin creams that contain certain ingredients to help soften the skin and loosen dead skin cells. These ingredients could include urea, lactic acid, glycolic acid (alpha hydroxy), salicylic acid, or tretinoin.
- Use steroid creams to reduce redness and itching.
It may be weeks or months before you see results of treatment, so be patient. Even if the bumps go away, keep your treatment plan going since keratosis pilaris often returns when treatment is stopped.
Living with keratosis pilaris
Here are some tips to help improve the appearance of your skin:
- Wash your skin gently. Avoid scrubbing the affected area. Use warm (not hot) water and a mild soap (some brand names: Cetaphil, Lubriderm, Purpose). Avoid deodorant or soaps with a strong fragrance because the perfumes used in these products can dry out your skin.
- Pat dry your skin after showering or bathing while being careful not to rub.
- Use a moisturizer after every shower or bath. Apply it within 5 minutes of getting out, while your skin is still damp.
- Apply moisturizer 2 to 3 times a day. Moisturizers that contain urea (some brand names: Eucerin, Lubriderm) are especially helpful because they soften dry, rough skin.
- Use a humidifier to increase the humidity of your environment.