What is paronychia?
Paronychia is a skin infection around the fingernails or toenails. It usually affects the skin at the base (cuticle) or up the sides of the nail. There are two types of paronychia:
- Acute: comes on suddenly and may not last long; it usually occurs on fingers.
- Chronic: lasts longer and may occur on your fingers or toes. It either doesn’t get better or keeps coming back.
Paronychia can happen to adults and children. Usually it isn’t serious and can be treated at home.
What are the symptoms of paronychia?
Typically, paronychia begins with pain, swelling and redness around the base or the sides of the nail. Acute paronychia can cause pus-filled pockets (abscesses) to form.
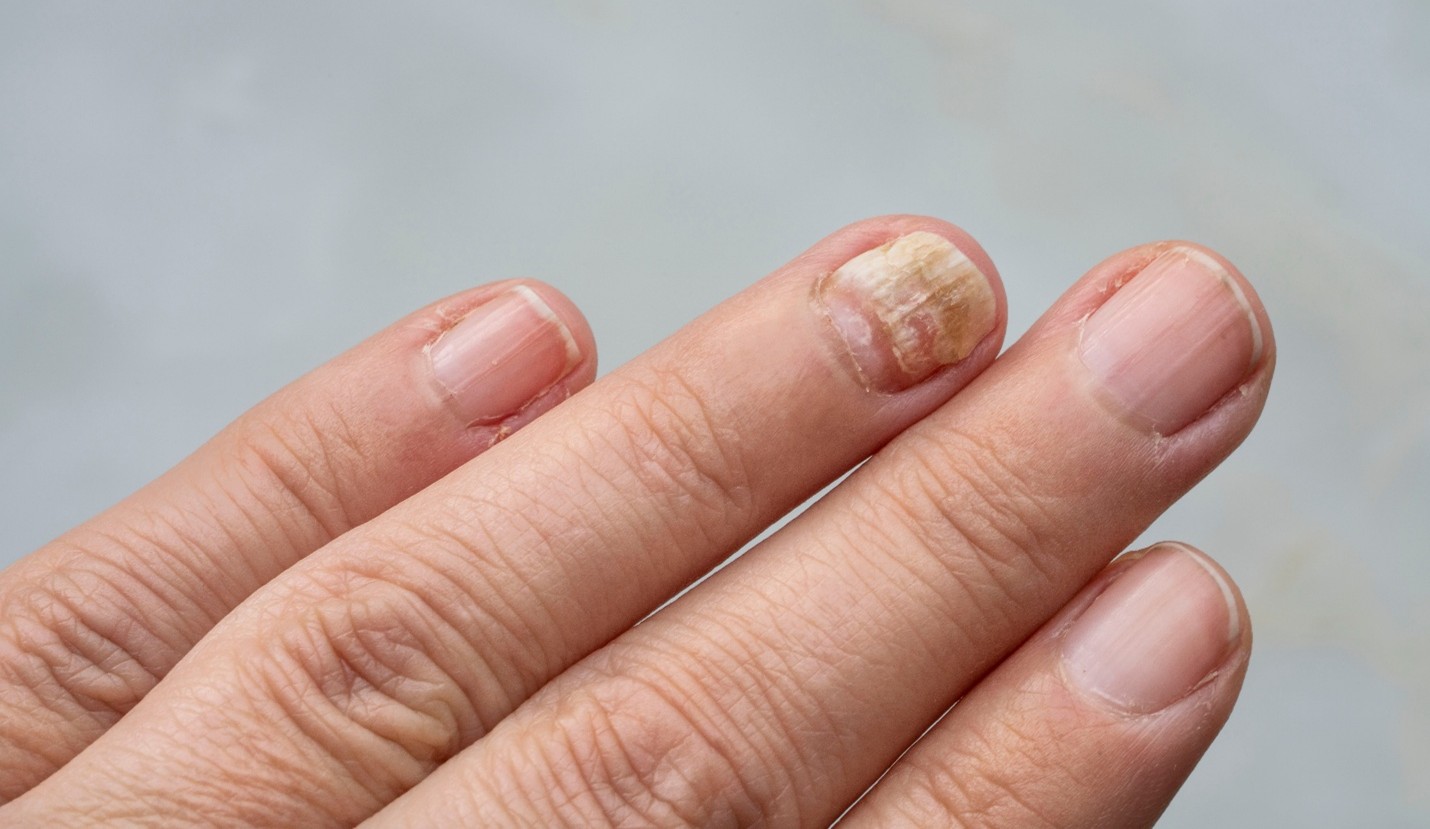
Chronic paronychia may cause the cuticle to break down. This type of paronychia may eventually cause the nail to separate from the skin. The nail may become thick, hard, and deformed.
Paronychia caused by bacteria can get worse quickly. Fungus-caused paronychia typically gets worse slowly over time.
What causes paronychia?
Paronychia happens when the skin around the nail gets irritated or injured. Germs get into the skin and cause an infection. These germs can be bacteria or a fungus.
Often, the skin is injured because of biting, chewing, or picking at the nails. It can also be caused by pulling hangnails or sucking on fingers. An ingrown toenail can also cause paronychia.
Moisture allows certain germs, such as candida (a type of fungus) and bacteria to grow. People whose hands may be wet for long periods of time are at higher risk for chronic paronychia. These may include bartenders, dishwashers, food handlers, or housecleaners. Chronic paronychia may also be caused by irritant dermatitis, a condition that makes skin red and itchy. Once the skin is irritated, germs can take hold and cause an infection.
Paronychia is more common in adult women and in people who have diabetes. People who have weak immune systems are also at higher risk of getting paronychia. This includes people who must take medicine after having an organ transplant or people who are infected with HIV.
How is paronychia diagnosed?
Your doctor can diagnose paronychia with a simple physical exam. Special tests aren’t usually necessary. Your doctor may want to send a sample of fluid or pus to a laboratory. There they can identify the bacteria or fungus that is causing the infection.
Can paronychia be prevented or avoided?
Nail and Cuticle Care Tips
The best away to avoid acute paronychia is to take good care of your nails.
- Avoid injuring your nails and fingertips.
- Don’t bite or pick your nails.
- Keep your nails trimmed and smooth.
- Avoid cutting nails too short.
- Don’t scrape or trim your cuticles, as this can injure the skin.
- Use clean nail clippers or scissors.
How to Prevent Chronic Paronychia
You can avoid chronic paronychia by keeping your hands dry and free from chemicals. Wear gloves when working with water or harsh chemicals. Change socks at least every day, and do not wear the same shoes for two days in a row. This allows them to dry out completely.
Paronychia treatment
Paronychia treatment methods depend on how severe the infection is.
Home Remedies for Mild Paronychia
If you have acute paronychia, soaking the infected nail in warm water 3 to 4 times a day can help reduce pain and swelling. It should heal up in a few days.
Medical Paronychia Treatments: Antibiotics and Antifungals
If the infection is very painful, doesn’t get better with home care, or has a pus-filled abscess, you may need to see your doctor. Your doctor may prescribe antibiotics if your paronychia is caused by bacteria. He or she may prescribe antifungal medicines if your infection is caused by a fungus.
Drainage and Advanced Care for Severe Cases
If you have an abscess, your doctor may need to drain it. Your doctor will numb the area, separate the skin from the base or sides of the nail, and drain the pus.
If you have chronic paronychia, it is important to keep your nails dry and protect them from harsh chemicals. You may need to wear gloves or use a skin-drying cream to protect skin from moisture. You may need an antifungal medicine or antibiotic, depending on what is causing the infection.
Paronychia caused by a fungus can be hard to get rid of. Be patient and follow your doctor’s recommendations. If the infection does not clear up, be sure to tell your doctor.
Living with paronychia
Most of the time, paronychia treatment is effective. But sometimes complications can happen.
Rarely, paronychia can cause permanent damage to your nail. If you have diabetes, there’s a risk that paronychia could spread to deeper tissues and bones, or into the bloodstream and other parts of the body. In extreme cases of deep infection, paronychia can result in the loss of fingers, toes, or limbs.
Be sure to contact your doctor if:
- Treatment doesn’t help your symptoms
- You have a fever or chills
- Red streaks appear on your skin, running from the infected area toward your body (for example, up your foot from your toes or up your hand or wrist from your fingers)
- You have joint or muscle pain