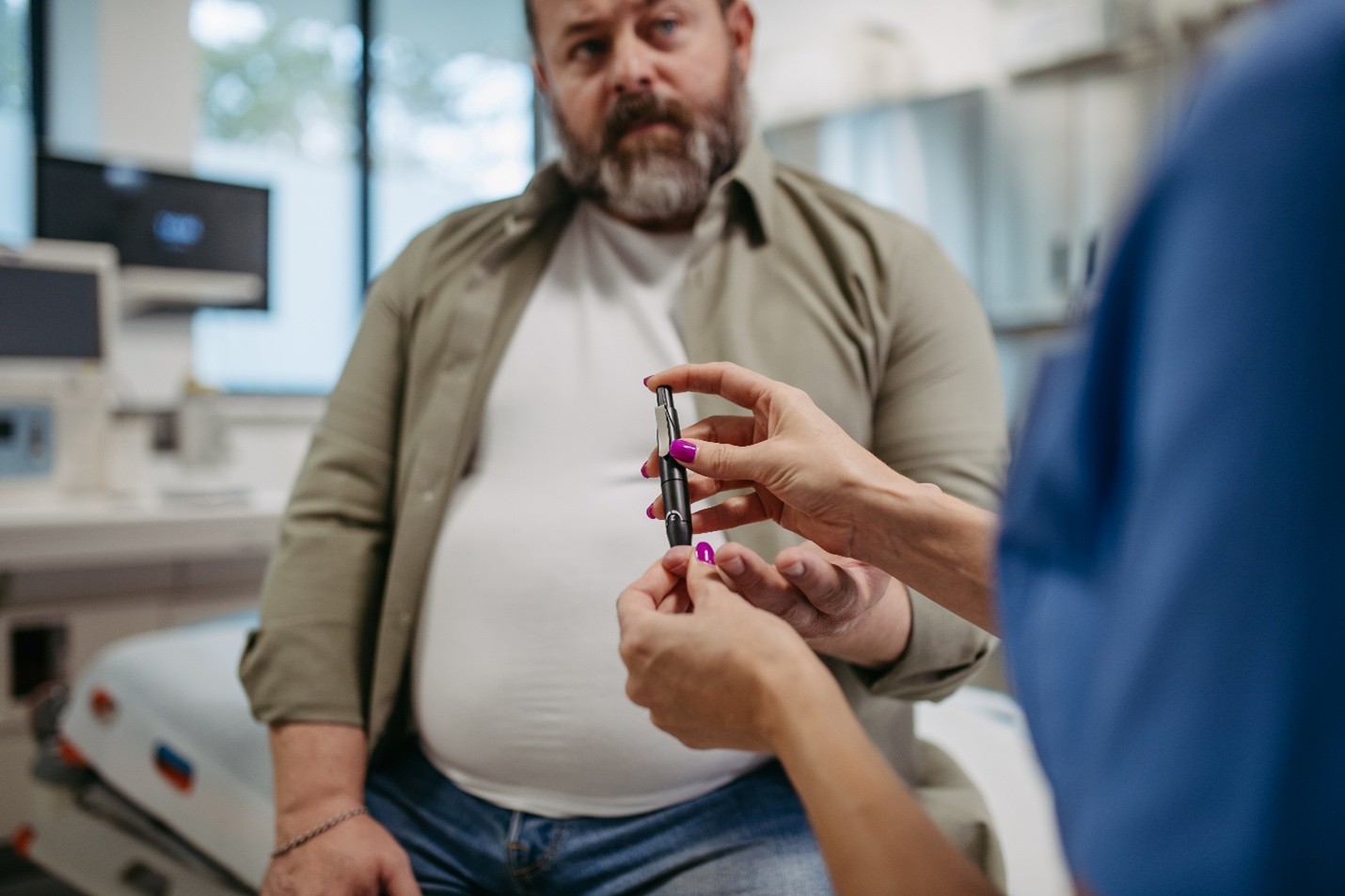
What is type 2 diabetes?
Type 2 diabetes is a disease that occurs when your blood sugar is too high because your body can’t regulate the sugar. Blood sugar is called glucose, and it is your main source of energy that comes from the food you eat. A hormone called insulin is required to help glucose enter your cells to be used for energy. With type 2 diabetes, your body doesn’t produce enough insulin or doesn’t use insulin as it should, causing blood sugar levels to rise.
Type 2 diabetes typically develops in middle-aged and older adults but is increasing in children and young adults. Type 2 diabetes is the most commonly diagnosed type of diabetes. If it’s left untreated, it can cause serious health problems.
What causes type 2 diabetes?
Type 2 diabetes usually progresses slowly over time. It starts with insulin resistance. This is a condition in which your cells don’t respond normally to insulin. Type 2 diabetes may be caused by several factors, including:
- Being overweight and having obesity
- Not being physically active
- Genetics and family history
Symptoms of type 2 diabetes
The symptoms of type 2 diabetes can be so mild that you might not even notice them. For others, symptoms of diabetes may include:
- Feeling very thirsty
- Feeling very hungry
- Feeling extremely tired
- Urinating (peeing) more often
- Blurry vision
- Numbness, pain or tingling in the feet or hands
- Sores that do not heal
Type 2 diabetes causes and diagnosis
You are at a higher risk of developing type 2 diabetes if you are overweight and are not physically active. If you have family members with type 2 diabetes or are of a certain race or ethnicity, you may also have an increased risk of developing the disease. Certain health conditions, such as high blood pressure and high cholesterol, can also lead to type 2 diabetes.
Your family doctor can diagnose type 2 diabetes through different blood tests. The hemoglobin A1C test (A1C test) is a very common blood test used to measure your blood sugar, or blood glucose, over a period of time. Your family physician will also ask questions about your health and family history.
How to manage type 2 diabetes
Your health care team will help you create a plan to manage your diabetes that is specific to you. The key to successful diabetes management is living a healthy lifestyle and regular follow-up with your family doctor. Start a healthy eating plan by understanding how different foods can affect your blood sugar. Living with type 2 diabetes does not mean you can’t enjoy the foods you love, but you will need to consider portion sizes, nutrition labels and the timing of your meals. Incorporate physical activity or exercise into your daily routine. If you smoke, work on quitting.
You may need to check your blood glucose levels regularly, and your doctor will tell you how often to do it. Even if you do not use insulin, checking your blood glucose level can help you manage your type 2 diabetes. If you take oral medicine to control your diabetes, you must ensure that you take it as prescribed. It is also important to regularly monitor your blood pressure and cholesterol levels through your family doctor. By taking these important steps, you can reduce the risk of diabetes-related health problems.
DKA
Over time, uncontrolled diabetes can cause severe damage to your heart, kidneys, feet, eyes and skin. Although rare, if left untreated type 2 diabetes could lead to a life-threatening condition called diabetic ketoacidosis (DKA). DKA is caused by too many ketones, which are chemicals, in the blood. High levels of ketones act as a poison to the body. People with DKA can have the following symptoms:
- Extreme nausea or vomiting
- Frequent urination (peeing)
- Abdominal pain
- Deeper, faster breathing
- Confusion, weakness or dizziness
- Fruity odor on breath
- Dry or flushed skin
- If you suspect that you or someone you know is going into DKA, seek emergency medical treatment immediately.
How to prevent type 2 diabetes
The good news is that you can prevent and avoid type 2 diabetes through simple, healthy lifestyle choices.
- Lose weight. If you are overweight or have obesity, your health care team can help recommend ways to manage your weight.
- Move more. Any form of regular physical activity or exercise can help improve overall health and prevent a rise in blood sugar or blood glucose.
- Eat healthy foods. A balanced diet including all major food groups combined with smaller portions will help keep your blood sugar at the right level.
- Get enough sleep. Getting enough sleep can help balance blood sugar, improve mood and increase energy levels.
Frequently asked questions about type 2 diabetes
Can you reverse type 2 diabetes?
Exciting new research shows that type 2 diabetes can be reversed through medication and lifestyle changes. You also may be able to prevent or avoid type 2 diabetes through healthy lifestyle choices.
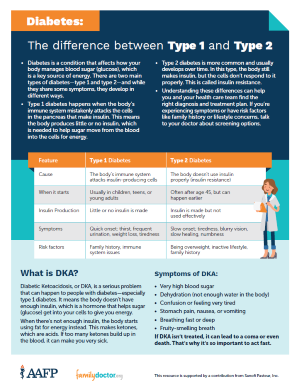
What’s the difference between type 1 and type 2 diabetes?
Type 1 diabetes is an autoimmune disease, which means that it is a disorder of your immune system. A person with type 1 diabetes cannot produce insulin. Type 2 diabetes is not an autoimmune disease and occurs when your body doesn’t produce enough insulin or doesn’t use insulin as it should.
Is diabetes mellitus type 1 or type 2?
Diabetes mellitus is simply the official medical term for diabetes. The term diabetes mellitus can refer to type 1 or type 2 diabetes.
Do people with type 2 diabetes take insulin?
You may take oral pills or medicine that you inject under your skin, such as insulin. Insulin is a hormone produced by the pancreas that helps glucose enter cells. A person with type 2 diabetes may be prescribed insulin if the body doesn’t use insulin as it should.
Can you have type 1 and type 2 diabetes?
You cannot have both type 1 and type 2 diabetes. Type 1 and type 2 diabetes are different in the way that the body produces and uses the hormone insulin.
Questions to ask your doctor
- What is the best way for me to avoid long-term problems from diabetes?
- Is there any specific exercise that would be better for me to control my blood sugar?
- I have a really hard time with needles. Are there other ways to treat my diabetes instead of insulin?
- It’s sometimes overwhelming to have diabetes. Are there groups or other people with diabetes that I can talk with about this?
- I really enjoy sugary foods and so don’t think I can eliminate all sugar from my diet. Is there anything I can still safely eat?
ADVERTISEMENT
ADVERTISEMENT