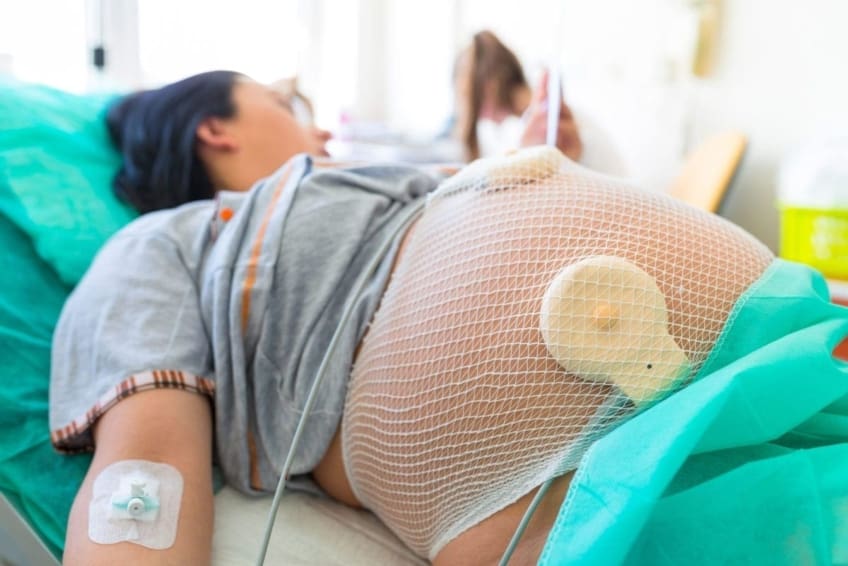
Your baby’s heart rate is usually monitored during labor. This is called fetal heart rate monitoring. It is done to keep track of your baby’s heart rate. Your doctor uses special equipment to listen to the baby’s heartbeat. This helps the doctor detect problems with the baby if they develop. It also helps reassure the doctor and you that labor and delivery are going normally.
Path to improved health
Your doctor will want to monitor your baby during labor. The easiest way to do this is through fetal heart rate monitoring. He or she can see how your baby is handling contractions. It helps them make sure the baby is doing okay.
Your doctor can monitor the baby either externally or internally. Externally means the sensors that monitor the baby are outside of your body. Internally means the sensors are put inside your body. Most women are monitored externally. Internal monitoring can be used if there is cause for concern or the doctor needs more exact information.
External monitoring
The simplest form of monitoring is called auscultation. This is a method of listening to the baby’s heart rate periodically. Your doctor will use a special stethoscope or a device called a Doppler transducer. He or she will press the device against your abdomen to listen to the baby’s heartbeat. They will do this at set times during labor, such as every 30 minutes. If you are at risk of having problems or if problems develop during labor, you will be checked more often. Some women prefer auscultation because it gives them the freedom to move around during labor.
The most common form of monitoring is external electronic fetal monitoring. This is when sensors are strapped to your abdomen. The baby’s heart rate is monitored continuously. Instruments record both the baby’s heartbeat and your contractions. This helps your doctor see how your baby is responding to the contractions. The recording doesn’t stop. Your doctor can check it at set times and see how labor has been going overall. The sensors remain on your abdomen for all of labor. You usually need to stay in the bed most of the time.
Internal monitoring
In this method, an electrode attached to a wire is placed directly on the baby. This monitors the heartbeat. A sensor is strapped to your leg. The electrode is threaded through your cervix and into the uterus. There it is attached to your baby’s scalp. A small tube can also be inserted to measure contractions. The two can provide more accurate measurements of your baby’s heartbeat and your contractions.
This kind of monitoring is usually done if the external monitor isn’t picking up well. This could be because you are moving around a lot, or if you have obesity. Your doctor may want a more accurate reading for other reasons. These could include risk factors or possible complications. This method can only be used if your cervix is dilating and your water has broken.
Pros and cons
Some women don’t want to be continuously monitored. You can’t move around with it. It takes away options for pain relief during labor, such as walking. Yet many doctors want you to do it. Your wishes could affect where you choose to have your baby. For example, you won’t have electronic fetal monitoring in birthing centers or at home. If you don’t want continuous monitoring, talk to your doctor as soon as possible.
Fetal monitoring can sometimes detect a problem when there isn’t one. If it shows an irregularity, your doctor may decide your baby needs to be delivered sooner. He or she could recommend giving medicine to speed up labor. Or they could use forceps (with patient’s consent) or a vacuum-assisted delivery. But sometimes the irregularity could actually be indicating nothing. Then the baby is born sooner and with assistance for no reason.
What kind of monitoring do I need?
Auscultation is generally considered an acceptable form of monitoring if:
- Your pregnancy is low-risk.
- You haven’t had complications during labor.
You will need continuous monitoring if:
- You have a high-risk pregnancy.
- Complications develop during labor.
- You have an epidural for pain.
- You have to have medicine (oxytocin/Pitocin) to induce or speed up labor.
Things to consider
What is considered normal for my baby’s heartbeat?
Indications that everything with the baby is fine include:
- Heartbeat between 110 and 160 beats per minute.
- Heart rate increases when baby moves.
- Heart rate increases during contractions.
- Heart rate returns to normal after baby moves or after a contraction.
- Your contractions are strong and regular during labor.
What is not normal for my baby’s heart rate?
Signs that there could be a problem include:
- Heartbeat is less than 110 beats per minute.
- Heartbeat is more than 160 beats per minute.
- Heartbeat is irregular, or doesn’t increase when baby moves or during contractions.
What if my doctor detects a problem?
Changes in heart rate do not necessarily mean there is a problem. Some are natural, such as it increasing when your baby moves or during a contraction. These changes are considered signs of well-being in your baby. If your baby’s heart rate is very rapid or dips down, there are some simple changes your doctor may suggest:
- Changing your position.
- Giving you more fluids through an IV.
- Giving you supplemental oxygen.
Other things your doctor could do include:
- Stopping oxytocin if you’ve been receiving it.
- Giving you medicine to relax your uterus. This decreases your contractions.
- Infusing sterile fluid into your uterus if your water has broken.
If none of these interventions help, your doctor may consider speeding up delivery. To do this, you could have an assisted delivery. Your doctor uses forceps or a special vacuum to pull your baby out instead of waiting for the contractions to push him out. Or they may suggest you have a c-section.
Questions to ask your doctor
- Do you require fetal heart rate monitoring during labor?
- What are the advantages and disadvantages of it?
- Do I need continuous electronic fetal monitoring?
- Why would I need internal monitoring? How is this performed?
- What happens if my baby’s heart rate is abnormal?
![]()
Copyright © American Academy of Family Physicians
This information provides a general overview and may not apply to everyone. Talk to your family doctor to find out if this information applies to you and to get more information on this subject.







