As a health care worker, you may be exposed to sources of infection. These may be transmitted in three ways. First, you can come into contact with an infected person’s blood or body fluids. This also includes droplets from a cough or sneeze. You can come into contact with infectious materials. The last way infections are spread is through the air.
Path to improved health
You can protect yourself from infection by:
- Following the infection control guidelines in your workplace.
- Using protective gear, such as gloves, goggles, and/or masks.
- Treating all blood and body fluids as though they are infectious.
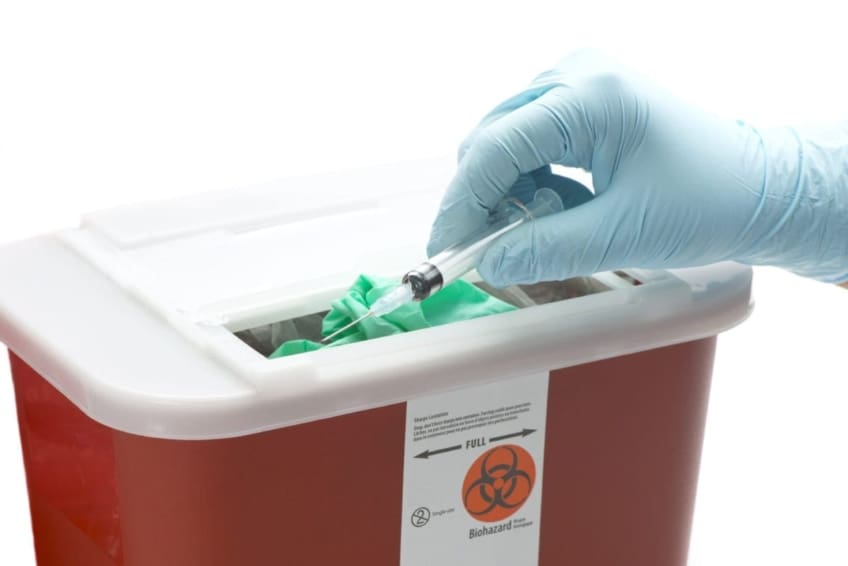
- Handling and disposing of needles and sharp instruments correctly.
- Getting immunized for necessary vaccines.
Infections and diseases can spread through certain body fluids. The main sources are blood, vomit, semen, vaginal discharge, breast milk, and pus. Internal fluids, like those from the lungs, heart, or stomach, also can transmit disease. Clear fluids, such as tears, saliva, sweat, and urine, contain little or no threat for infection. They cannot transmit infection unless mixed with blood.
For a skin or mucus splash, your risk is lower. Exceptions are if your skin has a wound, rash, or crack. Also, if the blood or fluids splash into your mouth or eyes. For a needlestick injury or cut, your risk is higher. In all cases, wash the affected area and get medical care right away.
A doctor will assess and test you for infection. They also may want to test the infected person (source).
- If the source has HIV, you may need to take preventive medicines. These should be started within hours of the incident.
- If the source is infected with hepatitis B, you will get hepatitis B immune globulin. This is if you haven’t been immunized or don’t have immunity.
- If the source has hepatitis C, you may need antiviral medicines.
- If the source has syphilis, you’ll be treated with antibiotics.
You may need follow-up or repeat testing to check for infection. This will depend on the source and the type of disease.
Things to consider
Some infections are more serious, including HIV, hepatitis B and C, and syphilis. However, you should protect yourself against all infections and viruses. To help with this, you can get vaccines.
If you haven’t had chickenpox, you should have a blood test. It will check your immunity to varicella, the virus that causes chickenpox. Most adults are immune, even if they haven’t had chickenpox. If you aren’t immune, you should have the 2-shot varicella vaccine series. Without the vaccine, you’re at risk of getting chickenpox and spreading it to others.
In rare cases, people can get chickenpox a second time. This can happen even if you’re immune to varicella. Chickenpox is usually milder the second time. If you get it again, tell your work so you can avoid contact with patients.
A Tdap vaccine is routinely given at age 11 or 12. It protects against tetanus, diphtheria, and pertussis (whooping cough). Pertussis is responsible for some coughs or cases of bronchitis that last longer than the usual cold. If your cold lasts more than 2 weeks, talk to your doctor. Pertussis can be life threatening to unimmunized infants. Anyone who did not receive the Tdap vaccine as a child should get it as soon as possible. Health care workers should get the Tdap booster for tetanus and diphtheria once every 10 years.
It’s important to know which patients might have tuberculosis. Those who are homeless or have immigrated from certain countries are at higher risk. They will have a chronic cough that lasts for weeks and brings up mucous or blood. They also may have fever, night sweats, or weight loss. You can catch this disease by breathing in droplets that get into the air when an infected patient coughs. Wear a protective mask if you work around patients who have tuberculosis. Infected patients also should wear masks to contain the infection. In an office setting, move them out of the waiting room. In a hospital setting, put them in isolation.
Questions to ask your doctor
- What other vaccines should I get to avoid infections at work?
- If I’m exposed to blood or body fluids in my workplace, what are the chances I will get infected?
- When and how will I know for sure if I’m infected?
Resources
National Institutes of Health, MedlinePlus: Infection Control
U.S. Department of Labor, Occupational Safety and Health Administration: Infectious Diseases
![]()
Copyright © American Academy of Family Physicians
This information provides a general overview and may not apply to everyone. Talk to your family doctor to find out if this information applies to you and to get more information on this subject.







